What is CAMS?
Evidence-Based Treatment
Patient-Centered Approach
Easy-to-Implement
Decreasing Malpractice Liability
Cost-Effective Care
Easy-to-learn suicide-focused treatment rooted in collaboration and backed by evidence.
The Collaborative Assessment and Management of Suicidality (CAMS) is an evidence-based approach to treating people suffering from serious thoughts of self-harm. The provider and patient collaborate using tools such as the Suicide Status Form. Together, they identify and address the “drivers” — the root causes behind the patient’s suicidal thoughts.
Whether you’re a seasoned clinician or an aspiring mental health student, the CAMS Framework equips you with the skills to effectively reduce someone’s suffering and treat suicidal risk.
Evidence-Based Treatment
Built on 40 years of ongoing clinical research, the CAMS Framework is an empirically-validated treatment application of suicide-focused care. The effectiveness of CAMS has been recognized and supported by the CDC, Joint Commissions and Surgeon General, as well as 11 clinical trials, 7 published randomized control trials, and 2 meta-analyses.
CAMS is referenced in the 2024 National Suicide Prevention Strategy and Federal Action Plan and Zero Suicide Toolkit. It has been integrated into many Zero Suicide initiatives worldwide.
Patient-Centered Approach
CAMS guides providers and patients to work as active collaborators, moving away from the traditional adversary model. Together they develop treatment and stabilization plans based on trust and mutual understanding–an approach that leads to positive patient feedback and better clinical outcomes.
Easy-to-Implement
We customize our training offers to your needs. With our integrative training models, you’ll master adherence with your first patient in as few as 4 sessions.
Decreasing Malpractice Liability
As a clinician, defending yourself in a malpractice lawsuit for wrongful death can be a painful and costly undertaking, particularly if the case goes to trial. A judgement against the provider can be hundreds of thousands of dollars (which also drives up malpractice insurance). Such lawsuits are incredibly stressful and often impact providers both personally and professionally.
The CAMS Framework offers thorough and comprehensive documentation that is a provider’s best safeguard from malpractice litigation. Moreover, using an evidence-based and suicide-focused treatment like CAMS is a provider’s best possible risk management strategy (Jobes & Barnett, 2024). Together with the patient, you will be completing the Suicide Status Form which can serve as the essential medical record for this proven approach to suicide-focused care.
Using a suicide-focused treatment like CAMS is specifically called out in the 2024 National Strategy for Suicide Prevention and may reduce your risk for malpractice lawsuits.
Good documentation stops a lawyer in his tracks. CAMS and the Suicide Status Form has great documentation.
Skip Simpson
The Law Offices of Skip Simpson, one of the country’s leading lawyers in the field of suicide malpractice litigation
Cost-Effective Care
Outpatient treatment is highly effective and preferred for most individuals experiencing suicidality. CAMS reduces Emergency Department (ED) visits among certain subgroups, minimizing healthcare costs and enhancing overall patient experience and outcomes.
Systems of Care
We are passionate about creating patient-centered systems of care to effectively treat people experiencing serious suicidal thoughts.
Beyond identifying individuals experiencing suicidal thoughts, we believe treatment must also include public and community awareness, screenings, suicide risk assessments, non-demand caring contacts, technology platforms for care, psychosocial services, and around-the-clock support.
We’re all in this together.

The Zero Suicide Initiative
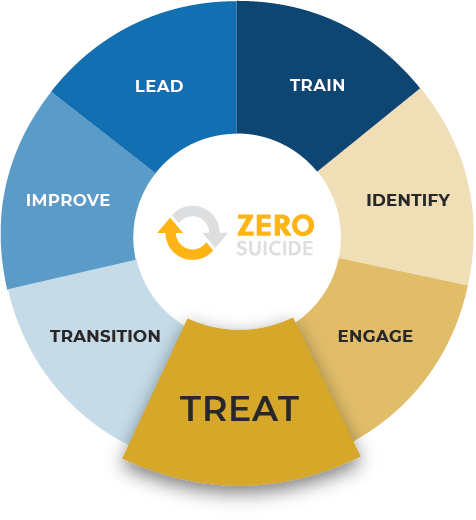
The Zero Suicide Initiative (Zero Suicide) aims to elevate suicide identification and care in healthcare systems. Since its 2012 launch and as part of the National Action Alliance for Suicide Prevention, Zero Suicide has shown notable reductions in suicide and suicide behaviors. It has also shown improvements to using evidence-based practices.
Zero Suicide promotes providers’ evidence-based practices by implementing seven core elements. CAMS specializes in training, identifying, engaging, and most importantly, treating.
Suicide Status Form (SSF)
The SSF is a unique, multipurpose clinical tool that guides the CAMS Framework.
Providers and patients sit side by side to collaboratively complete the form, identifying, planning for, and treating suicidal risk through various quantitative and qualitative assessments. This comprehensive document also serves as the medical record to reduce malpractice risk.
CAMS utilizes the SSF in three phases:
- Beginning (the index first session of initial assessment and treating planning)
- Middle (the interim sessions of CAMS that begin with SSF Core Assessments, focusing on treating suicidal drivers, and treatment plan updates)
- End (the final session of CAMS and the completion of the Outcome/Disposition SSF)





