On July 16, 2022, the United States took an enormous step forward in crisis care and suicide prevention with the launch of a nationwide 3-digit, 24/7 helpline, known as “988.”
In parallel with 911, the FCC designation of this easy-to-remember number for the Suicide & Crisis Lifeline (formerly the National Suicide Prevention Lifeline), marks an important shift in the way that suicidal thoughts and actions are prioritized, identified, and treated in the United States. And it’s already revolutionizing how individuals living with suicidal thoughts connect to life-saving resources across the US.
But it’s not enough.
The State of Suicide Treatment & Prevention in the US
In 2020, the CDC reported over 312,000 emergency visits for “self-harm injuries” and 45,979 suicide deaths, making suicide the 12th leading cause of death in the US. Suicide was the third leading cause of death for Americans ages 10-24 and the 12th leading cause of death overall.
There are 12.2 million adults and 3 million adolescents in the US with serious thoughts of suicide and yet current wait times for behavioral health care and the treatment of suicidal thoughts can be months. And unfortunately, the launch of 988 will not alleviate this crisis of care on its own.
According to the HHS Assistant Secretary for Mental Health and Substance Use, and leader of the Substance Abuse and Mental Health Services Administration (SAMHSA), Miriam E. Delphin-Rittmon, Ph.D., the demand for timely, effective mental health and suicide interventions is only going to increase — even as federal investment reaches an all-time high.
“Recent investments made in the [988] Lifeline have already resulted in more calls, chats, and texts answered even as volume has increased, but we know that too many people are still experiencing suicidal crisis or mental health-related distress without the support they need.”
In 2021, the National Suicide Prevention Lifeline received 3.6 million calls, chats, and texts. SAMHSA expects that number to at least double within the first full year after the 988 transition. According to Vibrant Emotional Health, call volumes to 988 are up 45% compared to the week before 988 went live and 66% compared to the same time in 2021.
How to Improve Suicide Treatment & Prevention at Scale
Creating an easy-to-use nationwide suicide prevention helpline is a fantastic tool that is already making a tangible impact on Americans’ lives. But 988 is just the first step in solving our national suicide crisis.
Suicide prevention and mental health crisis services will continue to overwhelm existing systems until we do these two things:
- Integrate evidence-based suicide treatment methods directly into the electronic health record (EHR) via the Suicide Status Form (SSF) so that every clinician has access to a simple, effective tool to assess and treat suicidal thoughts in a growing client population.
- Provide next-day suicide interventions across the country, regardless of location, with help from organizations like The Hope Institute.
Here’s how healthcare providers can build on the momentum of the 988 launch to create a better suicide response system and take the next steps in suicide treatment and prevention in the US.
Improving the Electronic Health Record with Evidence-Based Care
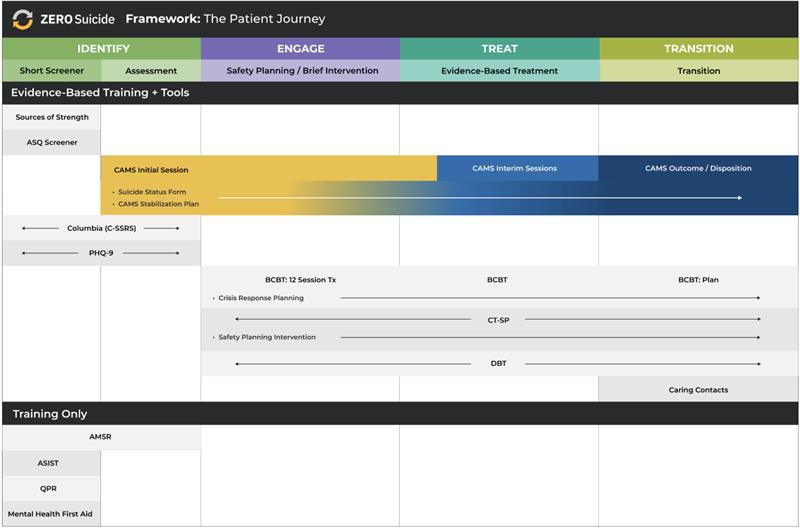
The biggest hurdle for effective suicide treatment and prevention in the US isn’t a lack of effective treatment models. In fact, the Collaborative Assessment and Management of Suicidality (CAMS) is one of four evidence-based treatments that are trusted by the Joint Commission, Surgeon General and the CDC.
CAMS itself has more than 30 years of evidence, five published randomized control trials, and two meta analyses one of which shows that CAMS is a “Well Supported” treatment by CDC criteria and is even proven to “reduce hopelessness and increase hope” in as few as six sessions.
So if the problem with suicide prevention isn’t a lack of effective treatment methods, what is the issue?
One of the biggest limiting factors in the US for improving suicide crisis care is the current Electronic Health Record (EHR) — or more accurately, the lack of evidence-based methods for suicidal treatment and prevention within most EHRs.
However, CAMS can change that with an 8-page form — the Suicide Status Form — that is a proven and reliable multi-purpose clinical tool once it’s included in the medical record.
How the SSF works
Simply put, the SSF functions as a clinical roadmap within CAMS for assessments, treatment planning, tracking ongoing risk, and clinical outcomes for suicidal ideation. It does this in three-parts:
1. Initial session (Pages 1-4)
The first session of CAMS includes a therapeutic assessment completed by the client and the clinician, and the development of a stabilization and a treatment plan for two “drivers” that the client says makes them consider suicide.
2. Interim (Pages 5 & 6)
In each interim session of CAMS, the clinician treats the client’s drivers and checks with the client to ensure the stabilization plan and treatment plan are working.
3. Outcome (Pages 7 & 8)
The final session of CAMS is held when the clinician and the client is behaviorally stable and able to manage suicidal thoughts and feelings.
Learn how to use the Suicide Status Form
The goal is to build the Suicide Status Form directly into the medical record itself, integrating this effective method into the diagnosis, treatment, and even the billing model for clients across the country for continuity of care no matter where you are. Meta analytic research has even shown that collaboratively completing the assessment portions of the SSF is a therapeutic experience for the client in itself.
One substantial obstacle to the adoption of this evidence-based treatment has been the lack of adoption of this tool into EHRs.
Fortunately, that’s changing as more healthcare record providers recognize the need for integrated systems that streamline assessments, guide treatment, and improve client outcomes within increasing client populations — especially at scale.
Who is currently using the SSF?
At CAMS-care we are proud to say that we have partnered with several healthcare leaders to include the SSF in their platforms and client records including:
- Epic
- Netsmart
- InSync
- Psyquel
- Bhworks – a School Mental Health Management System
- NeuroFlow – a leading Health Integration Solution
These Electronic Health Record and Health Management platforms recognize that having access to evidence-based care within clients’ records is essential for clinicians to meet the complex needs of growing client populations. And that need is quickly being felt as 988 rolls out across the country.
The first crucial step in improving suicide outcomes is to integrate an evidence-based framework — like CAMS and the Suicide Status Form (SSF) — directly into the electronic health record so that every clinician has access to tools backed by more than 30 years of clinical trial evidence.
The next step is changing the way we respond to suicide crises by providing interventions as quickly as possible — ideally within 24 hours of first contact.
The Importance of Next-Day Suicide Interventions
SAMHSA has created new federal resources to help states, territories, tribes, and mental health and substance use disorder professionals better respond to suicide crisis events, and 988 is a large part of that effort that will undoubtedly help millions of Americans.
However, treatment and prevention still largely occur at the state or local level, and that’s where 988 currently falls short.
Today, many suicide crisis interventions involve routing people to emergency departments where they can wait for hours—or even days—for treatment. The other alternative is waiting months for an appointment with a community mental health center (where care is typically not suicide focused or evidence-based). Obviously, neither of these is optimal.
Not only are most EDs ill-equipped to assess, treat, and track suicidal thoughts, they’re also unable to keep up with the increased demand from 988. Relying on either option to treat and prevent suicide leads to wasted resources, or worse, a lack of trust in the system from clients in desperate need of urgent care.
SAMHSA has designed a 988 crisis response system — a Mobile Crisis Team — for people who are in immediate danger to themselves. And while it’s essential that these systems are implemented, most people with serious thoughts of suicide don’t want or need to be picked up and taken to a Crisis Facility.
In fact, according to National Lifeline data, less than 10% of callers are high-risk cases that require immediate intervention on this scale.
The other 90% of callers to 988 can simply benefit from a trained crisis line specialist to provide a Safety Plan and a next-day appointment to receive evidence-based treatment that specifically addresses thoughts of suicide.
And the good news is there’s a way to integrate 988 with existing institutions, like the Hope Institute, to provide better, more timely suicide interventions at locations across the country.
How The Hope Institute works
The Hope Institute integrates the best practices of a modern crisis care continuum with next-day appointments, taking referrals from emergency rooms and hospitals and relieving the strain of suicidal distress on schools, colleges, jails, sheriff’s offices, and first responders. Even better, treatment begins within 24 hours of referral.
Outpatient or telehealth—sometimes offering multiple sessions per week based on need — further increases reach across strained healthcare networks and remote rural areas with few to no services.
Hope Institutes use a combination of evidence-based, suicide-focused treatments, including the Collaborative Assessment and Management of Suicidality (CAMS) and group skills in Dialectic Behavioral Therapy (DBT).
Moreover, Hope Institutes are small, calm, and stigma free, staffed by clinicians who focus exclusively on suicide cases. And the results are clear.
Hope Institute clients are stabilized in an average of 6 weeks (adolescents in an average of 5.2 weeks). Even more impressive, a Hope Institute can be opened in just 90 days and an 18 clinician center can treat over 3,000 clients each year.
Next Steps: How to Include CAMS in your EHR
988 is changing the conversation around suicide treatment and prevention. But there’s still a long way to go to improve suicide crisis care in the US.
It’s time to integrate evidence-based best practices into your EHR, and support more responsive, effective, targeted next-day suicide interventions to communities across the country at scale.
Contact our team today to learn more about the Suicide Status Form (SSF), how you can integrate evidence-based frameworks like CAMS into your EHR, or how to bring The Hope Institute into your community.
Derek Lee – derek@thehopeinstitute.net
Andrew Evans – andrew@cams-care.com
For more information about 988, our partners at NeuroFlow wrote a helpful blog post discussing the new hotline.
For training in evidence-based, suicide-focused treatment visit CAMS Training Products.